|
Data from the Vietnam Veterans Alzheimer’s Disease Neuroimaging Initiative Project (ADNI-DoD) was used. Both the MoCA and MMSE are frequently administered in clinical care settings and are advantageous given that they are quick, affordable, and can be administered in a broad range of settings. In the current study, we investigated associations between baseline PTSD symptom severity and longitudinal change in cognitive function using two widely used cognitive screeners in older adults, the Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA). The substantial benefits of reliable biomarkers for early detection of neurodegenerative disease underscores the need for additional research in this area. As such, an outstanding question remains whether the link between traumatic stress symptoms and cognitive decline is explained by elevated cerebrospinal fluid (CSF) AD biomarkers, or whether stress accounts for unique variance in cognitive decline among older adults. Despite these discrepant findings, the potential to use these biomarkers to detect early onset of AD indicates that additional work is needed to clarify the relationship between PTSD, biomarkers of AD pathology, and cognitive outcomes, particularly in samples without known neurodegenerative disease. For example, researchers have posited that lifestyle factors including sleep disturbance, inflammatory responses of the immune system, decreased cognitive reserve, and metabolic and vascular diseases may contribute to the relationship between PTSD and dementia. Discrepant findings may be due to additional mechanistic contributors to observed associations between PTSD and cognitive decline. 
Similarly, whereas one recent study found that PTSD did not increase risk of Aβ or tau burden using blood-based markers, another study found decreased plasma Aβ in World Trade Center responders with PTSD. By contrast, another study using PET imaging found that PTSD was indeed correlated with Aβ burden. Three recent positron emission tomography (PET) studies found that PTSD did not increase risk of Aβ or total tau (t-tau) burden. However, the results of human studies investigating the relationship between PTSD and AD biomarkers have been mixed. 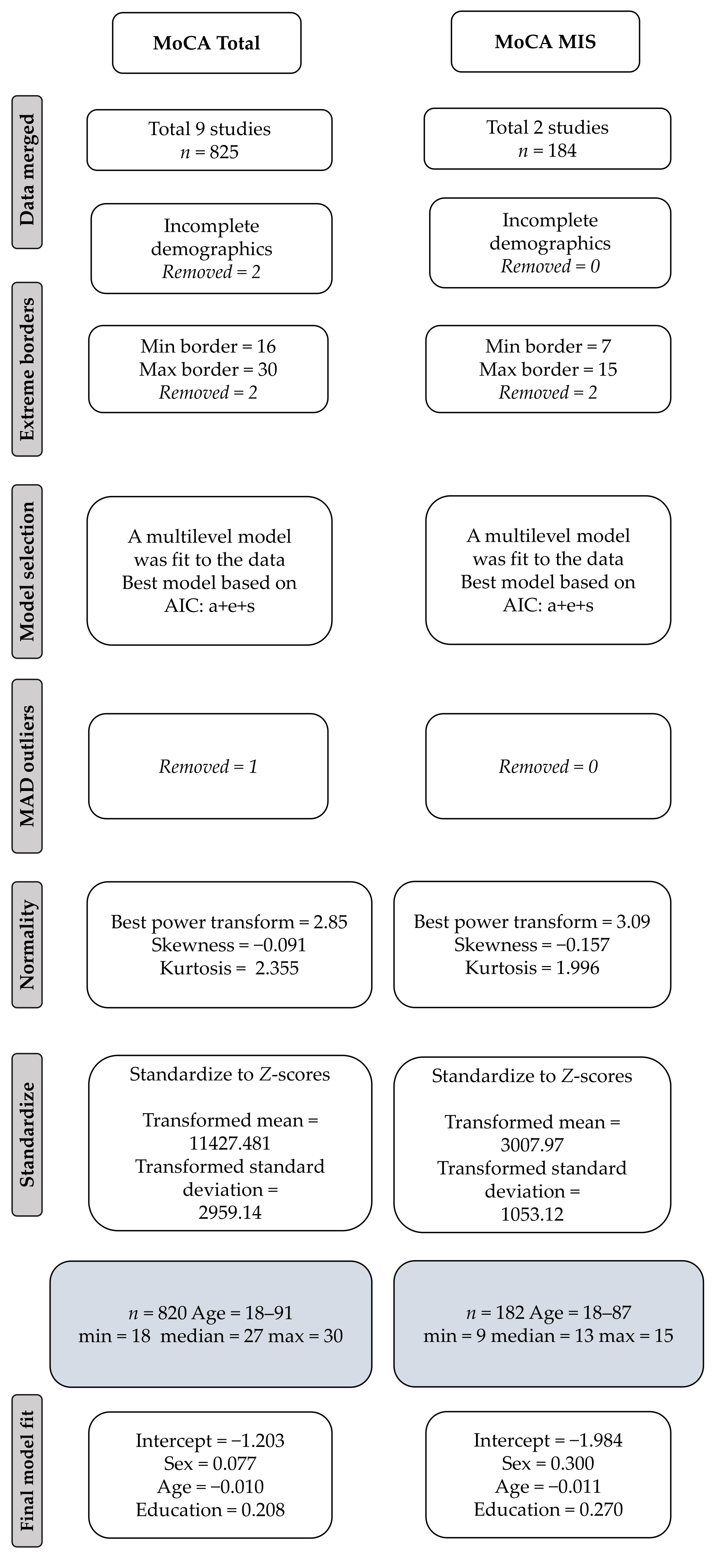
Preclinical studies have shown that stress accelerates Aβ and tau pathology through corticotropin-releasing factor (CRF) overproduction. The high prevalence of PTSD symptoms in populations such as military personnel underscores the need to understand the influence of PTSD symptoms on cognition in aging.Īlthough the mechanisms linking PTSD to Alzheimer’s disease (AD) and other dementias are unknown, there are several biological pathways that link stress with AD including neuroinflammation, metabolic disorders, and neuropathological markers such as beta-amyloid (Aβ) and tau. Studies have shown that patients with PTSD are twice as likely to develop dementia than those without PTSD, and a recent meta-analysis confirmed that PTSD is a strong risk factor for all-cause dementia. There is growing concern that PTSD confers elevated risk for mild cognitive impairment and dementia. 
PTSD has been linked with poorer performance on neurocognitive tasks across various domains including attention, working memory, processing speed, verbal learning and memory, and executive functions. Posttraumatic stress disorder (PTSD) is a chronic, debilitating condition characterized by symptoms including intrusive re-experiencing of a traumatic event, avoidance of reminders of the event, negative mood/cognitions, and hyperarousal. Treating PTSD should be considered instrumental to maintaining cognitive function as adults age. Taken together, PTSD symptom severity is associated with accelerated cognitive decline. These analyses survived multiple comparison corrections. 
Analyses indicated that PTSD symptom severity was associated with a greater decline on the MMSE ( p < 0.04) and MoCA ( p < 0.024) after adjusting for biomarkers of AD, notably on the attention scale of the MoCA and the memory index of the MMSE. In a preclinical cohort of Vietnam Veterans, we examined the relationship between posttraumatic stress disorder (PTSD) symptom severity, AD biomarkers of beta-amyloid (Aβ) and tau, and change in cognitive performance on two widely-used screeners, the Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA). Chronic stress is a risk factor for dementia but whether it explains unique variance in cognitive decline in older adults above Alzheimer’s disease (AD) biomarkers is unknown.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
